|
|
Map of New Jersey
|
Once you notice the oddity of salt water in the lower reaches of the Delaware and Hudson rivers, it gets easier to understand the current theory that southern New Jersey was once an island. Like Long Island, it was separated from the mainland by a sound, but in the Jersey case the sound silted up from Trenton to New Brunswick, creating a new peninsula of "West" Jersey by uniting the island with the mainland. The colony was named after the island of Jersey off the coast of England, a gesture for Sir George Carteret, who was given the American area out of gratitude for once sheltering the exiled royal brothers Charles II and James from Cromwell, in that other Jersey. Cape May was probably a second distinct island later joined to the larger one by the transformation of the silted ocean into the bogs of the Maurice River. Cape May started as a whaling community, populated by Quakers from New York and New England, who always maintained a social distance from the Philadelphia Yearly Meeting. The long Atlantic beaches of New Jersey now repeat the main geological process, with successive generations of barrier islands first heaved up by the ocean and then packed against the mainland, filling up the brackish bay. The cycle of forming and packing successive barrier islands takes about three hundred years before a new one starts. In a larger sense, the process consists of the former mountains of Pennsylvania crumbling into the ocean and then responding to wave action.
It's no mystery, therefore, why southern New Jersey is flat, broken up by turgid meandering streams which casually empty in either direction. The head of Timber Creek, which flows into Delaware, is only eight miles from the head of the Mullica River, flowing toward the ocean. During the Revolutionary War, the British found it too dangerous to sail up these winding creeks, since at any moment they might make a sharp turn and be facing a battery of cannon on the shore. An arrangement quickly grew up that buccaneers would build ships in the center of heavy oak forests and sail them out to Barnegat Bay, thence out one of the inlets of the barrier islands into the blue water. The financiers of Philadelphia, many of them with names now in the Social Register, would come from the rear, sailing up the Delaware River creeks, and walking the last mile or two to privateer headquarters on the Atlantic-flowing creeks. Auctions were conducted, in which the ships were examined, the captain interviewed, and the crew observed in target practice. If you bought a small share you would be rich when the ship returned; and if it never returned, well, you had to invest in a different one. New Jersey is indignant of the opinion that these privateers were mainly responsible for winning the Revolution, but given little credit for it. Many more British sailors were lost to the privateers than soldiers were lost to Washington's troops and the economic loss to Great Britain of the ships and cargoes eventually became serious. Since much of the profit from privateering was recycled into the American war effort by Robert Morris, the British found themselves facing an enemy much more formidable than just the ragged frozen troops at Valley Forge on the Schuylkill. Meanwhile, William Bingham was conducting a similar privateering operation in partnership with Morris but based on the island of Martinique, but that's another story.
In later centuries, the traditions and geography of the Jersey Pine Barrens suited themselves to smuggling and bootlegging during the era of alcohol Prohibition, and even after Repeal, high taxes on liquor kept bootlegging profitable. As late as the 1950s, there were divisions of FBI men prowling the woods of South Jersey, on the lookout for trucks carrying bags of cane sugar, or coils of copper tubing. After housing developments started to invade the forests, the hardball politics of South Jersey reflected a Mafia culture thought more characteristic of South Philadelphia. Near Vineland and Atlantic City, it isn't just a culture, it has the accent, because it also has some of the ancestry.
REFERENCES
| New Jersey, A Historical Account of Place names in the United States: Richard P. McCormick: ISBN-13: 978-0813506623 |
Amazon |

|
|
Fred Etherington
|
Thoughts about Fred Etherington
Since my induction into The Right Angle Club in 1997, Fred Etherington was always most supportive of me and through the years we became very good friends, in spite of the difference in our ages. In summer 2001, I gave a talk to the Club about 3 cities in Germany and Fred then recommended me for the honored 4 year Board progression, resulting in becoming President of the Club in 2004. During this time, Fred and his brother, Burt, were the Club's historians and we further bonded at the monthly Board of Control meetings. Also during this time, we would see Fred and his family each summer in Nantucket. I remember riding my bike down India Street and passing Fred's rental house every day. When he had been more mobile, he and his family (his wife, Frances, and daughters Susan and Laurie) would come to our place for our cocktail parties. He also invited us for cocktails in his garden. Not being a big drinker himself, he still made a special effort to have a bottle of wine and a pint of gin for us sinners when we went to his home. I remember his great WW II stories and his adventures in Iwo Jima. We missed seeing him the last couple of years in Nantucket, but Julie and I would drop in to see him and Frances at Beaumont whenever we could. Although he was restricted to bed, he was always alert and very positive in his life views. To sum it up, I want to quote something our Racquet Club waitress, Rosie, said to me later on the day of his memorial service. She said to me: "He was always such a gentleman, and I loved helping put on his Club pin". Fred and Burt, both proud Princetonians, were our two special Life Members and were such a big part of what made the Right Angle Club something very special and enduring. Fred had joined the Club in 1950, he was our President in 1958, and his memory lingers on for those who were fortunate enough to have known him over the many years he graced us with his kind wisdom and joyful presence.
Robert Bryan
Past President 2004

|
|
A Prisoner of the Stone
|
The first revolution in book authorship has already taken place. Almost all manuscripts arrive on the publisher's desk as products of a home computer. In fact, many publishers refuse to accept manuscripts in any other form. Not only does this eliminate a significant typing cost to the publisher, but it allows him to experiment with type fonts and book design as part of the decision to agree to publish the book. What's more, anyone who remembers the heaps of paper strewn about a typical editor's office knows what an improvement it can be, just to conquer the trash piles. To switch sides to the author's point of view, composing a book on a home computer has greatly facilitated the constant need for small revisions. An experienced author eventually learns to condense and revise the wording in his mind while he is still working on the first draft. However, even a novice author is now able to pause and select a more precise verb, eliminate repetition, tighten the prose. He can go ahead and type in the sloppy prose and then immediately improve it, word by word. The effect of this is to leave less for the copy editor to do, and to increase the likelihood the book will be accepted by the publisher. The author is more readily able to see how the book looks than he would have been with mere typescript.
It must be confessed, however, that a second revolution caused by the computer has already come -- and gone. Not so long ago, I once linked primary documents already on the Internet to the appropriate commentary within my blog. The idea was to let the reader flip back and forth to the primary sources if he liked, and without interrupting the flow of my supposedly elegant commentary. In those early days of enthusiasm, volunteers were eager to post source material into the ether, just asking for someone to read it eagerly. I had linked up Philadelphia Reflections to nearly a thousand citations when an invincible flaw exposed itself. Historians were eager enough to post source documents, but not so eager to maintain them. One link after another was dropped by its author, producing a broken link for everyone else. The Internet tried to locate something which wasn't there, slowing the postings to a pitiful speed. Reluctantly, I went through my web site, removing broken links and removing most links. Maybe linking was a good idea, but it didn't work. There is thus no choice but to look to institutional repositories for historical storage, and funding to pay for maintaining availability for linkage. It is not feasible to free-load, although only recently it had seemed to be.
This pratfall assumed technology would provide more short-cuts than in fact it would. A more difficult obstacle emerges after some thought given to the nature of writing history because it seems remarkably similar to Michelangelo's description of how to carve a statue. Asked how to carve, he said it was simple. "Just chip away the stone you don't want, and throw it away." Michelangelo saw statues as "prisoners of the stone" from which it was carved, while insights and generalizations of history emerge from a huge mass of unsorted primary documents. But there is a different edge to writing history. Uncomfortably often, the process of writing history is one of disregarding documents which fail to support a certain conclusion, often documents which send inconvenient messages to modern politics. Carried too far, de-selecting disagreeable documents amounts to attempting to destroy alternative viewpoints. By this view of it, what the author chooses to disregard, is then as important as what he chooses to include. Unless awkward linkages are consciously maintained in some form, they will soon enough disappear by themselves. It is a great fallacy to assume that ancient history can be isolated from current politics, or even to believe that history teaches the present. Often, it is just the other way around.
For years I have regarded HSAs as "term insurance", or one-year term-of-risk insurance. That's being mindful of the difference between term life insurance and "whole life" life insurance, and universally regarding whole-life as much superior. That's because so many people drop their term life insurance without collecting anything, so the dirty secret is most of the profit of term insurance comes from people dropping their policies. That doesn't sound so good, but it's a free country and people can drop insurance if they want to. Originally, it could be said the dropped policies are a safety feature of term insurance, protecting the company against people who might otherwise bankrupt them by failing to do the sensible thing. Or it could be said term insurance is just insurance, making no claim of generating income. These are reasonable positions, with no cause for attacking them. I'm really quite indifferent to this issue; the important feature to me is that whole life seems to generate more income, and HSAs are premised on earning more income. So why not have Lifetime HSAs and generate more income for everybody?
To go on with this thought, consolidating all of the pieces into a single company ought to generate more income, and put the decisions in the hands of experts instead of the common man. Efficiency and good management could be rewarded, expert actuaries could guide policy. It just has to be better. However, term HSAs are savings accounts, not life insurance, so there is not much loss in stopping deposits, nor many points to dropping the account. The risk of escheat is lessened by having the deposits guarded by a company who could be sued for stealing it; after all, lots of people do forget they have what they have, or where they put it. Yes, you do have to worry about excess overhead. Life insurance started a few blocks away from my medical office in Philadelphia, and high taxes made it move away. So, I have observed the Taj Mahal excesses, or even the Temple of Karmac excesses, of the former president's offices in those converted buildings. Nevertheless, I still have the strong feeling that whole life insurance generates greater efficiencies than term insurance does, and am attracted to the idea of consolidating the whole operation into a whole-life insurer -- instead of depending on millions of individuals to do the same thing, and competently handle what they are doing.
True, life insurance companies have armies of salesmen to persuade young folks to pay higher premiums than term insurance would require. The amount of premium for term HSAs would, however, have to approximate the $ 350,000-lifetime medical costs which the average American now sustains. Perhaps that's a good enough balance, particularly if it is front-end loaded.
What really bothers me is that it would take such a long time, perhaps 90 years, to prove that what you were doing had clear superiority. As I mentioned before, it puzzles me that whole life companies could survive long enough to establish the little rules of the game which make a difference between success and failure. True, they have enjoyed favorable tax treatment, but there is nothing new about that. Somehow, they figured out how to vindicate their methods in shorter time periods than a lifetime, even though they were undertaking lifetime risks. If some of them know the secrets, I hope they will step forward with proposals, but at my age, I'm not going to try to undertake such a risky voyage without a compass. Meanwhile, term HSAs are pretty darned good.
REFERENCE COMMITTEE A
When the idea of Last-Year insurance was presented to the AMA in December 1987, someone got to the microphone before I could. The AMA system is to publish meeting agendas in an advanced handbook. The subject had therefore been announced with a few spare sentences leading up to a proposal that the Association should look into the matter.
Whether the proposal was really unclear or whether a comedian just jumped at an opening, the subject was introduced with a mocking story. There was a little town outside Philadelphia, it seems, which used to have an ordinance about its fire hydrants. All hydrants were required to be inspected, one week before each fire. To follow that jibe with a description of insurance technicalities isn't the easiest position to in, but somehow the reference committee subsequently found the generosity to endorse the study.
Last year of life insurance is life insurance, paid after the death of the subscriber. The death benefit is paid to a health insurance company, reimbursement medical expenses incurred during the final year of the subscriber's life. The ultimate effect and the intention is to reduce the premiums of health insurance.
Since there can be no free lunch, it is clear this proposal will not reduce the cost of medicare care. The overall total cost of health insurance, therefore, is not changed by changing the form of premium collection. Indeed another layer of administration is required. What difference can it make whether you pay part of your premium to company A or company B? There are five answers.
Pre-Funding. As emphasized in the first section of this book, there is a great need to change our national system of health insurance from a pay-as-you-go system to a prefunded one. Such a radical shift in philosophy could be quite disruptive, so transitional steps are needed. each age group has a different point of view about pay-as-you-go. Young subscribers since their premiums are higher than their risks. Older subscribers feel thirty years of paying premiums creates a moral obligation for health insurance to carry them through their time of heaviest expenses. Consequently, established dominant health insurers have legitimate anxiety about new companies skimming off their healthy subscribers, leaving them with the sick ones and thus triggering an insupportable upward spiral of premiums and dropouts. The problem is to prevent this disaster for the private sector without precipitating it by changes which frighten away healthy subscribers. The problem is to fix the engine with the motor running.
Therefore, the initial reaction that last year insurance constitutes fragmentation is unfair; the segmentation is intentional, aimed at providing a gradual shift toward pre-funded health insurance in one area where it may be achievable. Ina segmented system, reducing the premium for a reduced unfunded component of health insurance means fewer remains at stake when you try to reduce the unfunded problem still further. Subscribers and insurers have more temptation but less latitude for gaming a system with fatal illness largely removed. When a greater proportion of claims represent randomized unpredictable acute illness or accidental injuries, the troublesome non-random risks are easier to see. The main difficulty is obstetrics, where family planning makes the insurance mechanism highly unstable; further ideas relating to obstetrics need to be developed and would be easier to develop if isolated underwriting of fatal illness proves a success.
Catastrophic Health Coverage. When Secretary of HHS Otis Bowen opened up the subject of catastrophic health insurance, he was probably as jolted as other physicians to watch the way this popular idea was instantly redefined. Once it became clear that catastrophic health coverage was a legislative slam-dunk, attempts were made to include domiciliary care of the aged, chronic illness of all sorts, mental retardation, and many other things which were expensive hence a catastrophe if you had to pay for them. Any hope Medicare could be restructured to pay for expensive illness first, paying for minor illness only if money was left over, went up in the smoke of special interest lobbying and revived hope among liberals of extending Medicare into a national health scheme.
This appalling example of what is out there on the other side of the gates, should at least remind serious students of health financing to use highly technical definitions when they make a proposal. There is, of course, plenty of room to argue that terminal care life insurance should cover expenses two years before death, or conversely that it should only cover two months. You can change the calendar definition of the coverage almost at will, and yet still intelligibly call it last-year insurance. The intent is clearly to cover the characteristically high costs of dying under medical supervision, as contrasted with saving lives with medical miracles, or nursing chronic invalids. if such coverage should pay for sunglasses, facelifts, or porcelain teeth, it would clearly be unintentional. Terminal care of fatal illness.
With the mechanism largely impervious to deliberate redefinition, and largely immune to manipulation for profit, isolation of the ethical issues of terminal care becomes a possibility. The cost of the problem gets held up for regular consideration, as premiums for the coverage get revised. Public attitudes about whether an extreme medical function is desirable would surely be reflected in the choices actually made between different coverage options. At different ages, one might feel a desperation to have every possible chance of survival, yet might later wish to be left to die in peace. Lawyers may argue about the legitimacy of living wills, but few would dispute that someone who spent his last-year insurance on something else, had made an important statement about his wishes. Deathbed discussions are almost invariably couched in slogans. The same relative, on the same day, may say "Let him die in peace," and then "Where there is life, there is hopes." Such expressions are usually made for the effect they have on the listeners and do not greatly illuminate underlying public attitudes about a serious subject. Observation of how much of their money they are collectively willing to spend is often a better guide to what people truly want that is the expression of opinion by their representatives. On one occasion, I happened to watch a large conf=gressional committee listening attentively to testimony on health insurance when unexpectedly the subject of euthanasia was introduced. Within two minutes, a majority of the congressmen had fled the room.
Pre-Existing Conditions. People change jobs with fair frequency, voluntarily and involuntarily. The tendency of young entrants into the job market is to take part-time or small-time employment in order to gain experience, but then if possible to work their way into permanent employment with a major employer. This progression is seen by them as moving into a better job, one "where the benefits are good."
This system has a sort of hidden equity to it since generous pay and generous benefits are definitely linked with the profitability of the firm. Unions have tended to be strong and aggressive in prosperous companies, while conversely companies in the rust belt losing out to foreign imports have found the industrial unions much more tolerant of givebacks. Fortune 500 companies definitely get a better quality of worker, because they pay up. With many exceptions, the tendency is to work for small struggling companies when you are young, and big prosperous ones when you get good at your work. This unofficial system provides health insurance directly to the working population, while the youngsters just entering the job market mostly don't have health problems. If such a young uninsured person does get suddenly sick, the larger companies may still pick up much of the cost involuntarily, courtesy of the cost-shifting mysteries within hospital accounting systems. Much against their will, the large prosperous companies do partially reinsure the system against risks being run within the pool of young people from whom their future employees will be drawn.
Obviously, such a system is unstable. One of its worst features is that those who develop extremely serious illness before they get into the employer health insurance mainstream, are probably permanently excluded from it. There is no way available to them or their parents to guarantee future insurability for health insurance. As long as health insurance remains so firmly linked to employment in a large firm, it is hard to imagine any solution except through modification of the life insurance mechanism. Even so, if large numbers of people are to be encouraged to protect their insurability for health insurance, some way must be found for them to get their investment back, once the huge majority of them eventually do acquire employer-paid health insurance. We will return to this issue in the next chapter.
If the average person lives to be 80, and that's almost true, only forty years of that time are spent in the workforce where employer-based group health insurance is the norm. Since this period of time includes the coverage of dependents children and has potential carry-over to retiree health benefits, it is critical for the individual worker and his family to lock up his health insurance protection. The most frightening aspect of sickness among active workers is the possibility they may not be able to get health insurance when they lose their jobs. To be sick and out of a job is to have a "pre-existing condition." Since the pre-existing condition is the one most likely to cause a problem, it is small consolation to be covered for everything else. To have a wife with leukemia or a child with cerebral palsy is a very strong reason not to switch jobs if there is any question of health insurance coverage. While the person who knows the condition exists may have some bargaining power or individual coverage options before he leaves the job. But to develop a serious health condition during a period of unemployment is a truly ominous situation. Insurance contracts do not include exclusions of coverage of pre-existing conditions as legal boilerplate, they really mean to exclude the risk to themselves. In fairness to them, it must be noted they cannot possibly allow people to get sick and apply for insurance. The situation needs some mechanisms for insuring against loss of health insurability, and last-year-of-life insurance might at least serve to reduce the range of potential uninsurability.
Portability. Our system of linking health insurance to the place of employment has the disastrous obverse that if you lose your job, you lose your health insurance. This particular issue periodically gets more attention when a recession in the economy leads to waves of layoffs. Employers of more than??? are required to maintain health insurance for ??? weeks after a layoff. Employees are entitled to continue their employer's group health plan at their own expense for ??? weeks more. However, such arrangements are complicated and unwelcome; it is not clear they are very popular with families who have suffered the bewilderment of losing their income. Last-year-of-life insurance would be as portable at your own expense, while funded life insurance is both portable and permanent as long as the cash values can carry the premium. Perpetual insurance is still better; the cash values have built to the point where the interest they generate is sufficient to pay the premium further contribution.
True, present income tax laws permit only term life insurance to be considered a business expense for an employer. In 1988 the Congress is undoubtedly in no mood for social legislation which increases the national budget deficit, such as by creating a tax shelter for cash-value life insurance. But laws can be changed when Congress wants to change them, and the experience with the catastrophic health insurance shows the public can sometimes whiplash congressional opinion very rapidly. A severe recession would immediately restore Keynesian ideas about budget deficits to fashion. The best present response to legislative defeatism on this subject is to examine the net effect on the deficit of replacing a portion of health insurance premiums with last-year life insurance premiums, transferring tax-deductibility from one to the other. If the two financial effects wash out, permitting last-year health premiums to be treated as business deductions should worry few practical politicians.
Experience-Rated Unfairness: The AIDS Epidemic.If a company had a policy of paying all medical bills of its employees, the cost to the company would vary with the amount of sickness there happened to be. Since self-insurance of this type represents at least half of all health insurance in America, health insurance companies must offer a comparable cost if they are to have any hope of selling insurance. Rather than establish a single premium rate for the community, the usual practice is to offer "experience rating", sometimes also called "merit rating." In an experience-rated group, the premium is adjusted up or down to reflect the cost of the claims actually submitted. From the point of view of the subscribing employer, the cost is the same as it would be to pay the claims directly, and the administrative profit of the insurance company may well be less than the cost of processing the claims in the employer's personnel department. Adjust this cost somewhat to recognize the interest earned or lost on the premiums and claims, and you pretty much have a formula for the dominant American health insurance system. The cost of fatal illnesses, the last year-of-life costs, are thus buried in a system which emphasizes the yearly costs of employers while making little analysis of the individuals who are included in the coverage.
From time to time, reformers have tried to force health insurance companies to charge a uniform community rate to all subscribers, but are immediately confronted with a rush by low-cost employers to drop out of insurance and adopt a self-insuring approach. As long as health insurance is unfunded and carries no future guarantees, it is not easy to convince lucky people they should pay more than they have to, just to lower the premiums of those who have bad luck. An earlier section of this book dealt with the pernicious effect on intergenerational risk-sharing which is exacted by the tax code in return for treating premium costs as business expenses. Many people see the wisdom of paying a higher premium when they are young and healthy so they will not be stranded when they are middle-aged and sick. A fair number of people are willing to pay more for their health insurance if remain healthy than if they happen to get sick. But almost no one wants to pay more for his health insurance when he is well while relying on the unenforceable voluntary generosity of future generations for support if he gets sick himself. Everyone distrusts the possibility that future generations might go self-insured and leave the present generation hanging out to dry.
Experience-rated health insurance, therefore, is an evil for which there are few obvious remedies. Since employment groups delimit final boundaries, experience-rating is inherent in basing health insurance on the employer. Last-year-of-life insurance contains the potential for the major cost risk of fatal illness to escape voluntarily from that employer-based partition. There is no way to know how much-hidden age, sex, race, or other discrimination there is in job recruitment, and certainly no. way to know how much the potential health costs are weighted in the equation. NOr is there any way to know how much American Business are unsuccessful with foreign competition because of these immeasurable issues is dramatically illustrated by the current epidemic of a contagious venereal virus, HIV...
AIDS is invariably fatal, its complications are expensive to manage, and it is relatively easy to surmise who is likely to catch it. This combination of features creates strong incentives for insurance companies to exclude the condition from coverage, or exclude high-risk groups from the subscriber base. Since the average cost of treating a single case is???, several HMOs have been driven out of business by having a run of cases of AIDS. From an insurance viewpoint, the most treacherous feature of AIDS is that the distribution of cases is not random throughout the population. If even a financially strong insurer is careless or altruistic about accepting high-risk groups, it's premium structure may rapidly become overpriced by comparison with competitors who somehow did not have so many cases. To be perfectly frank, homosexuals are overrepresented in the entertainment, fashion, and advertising industries, as well as the art world in general. It is almost impossible to imagine such industries maintaining an employment-based health insurance system in the future except if they somehow exclude paying for the risk of AIDS. If the epidemic spreads, and particularly if legislatures seek to prevent the exclusion of certain industries, then cities like San Francisco may simply not have any health HMOs or states like New York may not have any health insurance. Whether the exclusion is applied to people with positive blood tests, or to unmarried males, or to the entertainment industry, to cities or to whole states, insurers will find a way to protect their own solvency. If not, the whole country will be without health insurance until a cure is found.
Consider now the advantages of last-year-of-life health insurance for coping with this problem. Since AIDS is invariably fatal, it has the grisly advantage that no one is going to recover from the condition, only to contract a second expensive fatal illness later. Everybody else who doesn't get AIDS is also going to have a last year of life, and for the majority, it will be an expensive year. Medicare finds that ??% of its claims over the last 60 days of someone's life. Because the AIDS victims are young they have fewer years for compound interest to reduce premium costs, but having said that it remains true the population-wide risk of fatality at a young age is very small. Community premiums could double or triple without discouraging potential subscribers who have the cost of terminal cancer in mind. Actuarial costs of last-year insurance for the whole population can be calculated much more accurately than any individual can guess his own risk. Risk-avoidance strategies might somehow evolve, but with so little annual mortality in employer groups, yearly experience-rating could not be their mechanism.


 Originally the "lower counties" of Pennsylvania, and thus one of three Quaker colonies founded by William Penn, Delaware has developed its own set of traditions and history.
Originally the "lower counties" of Pennsylvania, and thus one of three Quaker colonies founded by William Penn, Delaware has developed its own set of traditions and history.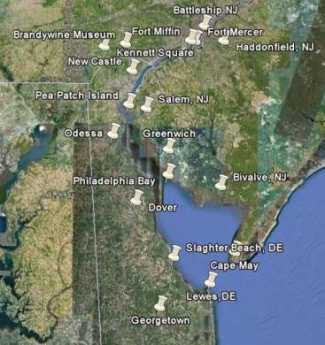 Start in Philadelphia, take two days to tour around Delaware Bay. Down the New Jersey side to Cape May, ferry over to Lewes, tour up to Dover and New Castle, visit Winterthur, Longwood Gardens, Brandywine Battlefield and art museum, then back to Philadelphia. Try it!
Start in Philadelphia, take two days to tour around Delaware Bay. Down the New Jersey side to Cape May, ferry over to Lewes, tour up to Dover and New Castle, visit Winterthur, Longwood Gardens, Brandywine Battlefield and art museum, then back to Philadelphia. Try it! Millions of eye patients have been asked to read the passage from Franklin's autobiography, "I walked up Market Street, etc." which is commonly printed on eye-test cards. Here's your chance to do it.
Millions of eye patients have been asked to read the passage from Franklin's autobiography, "I walked up Market Street, etc." which is commonly printed on eye-test cards. Here's your chance to do it. In 1751, the Pennsylvania Hospital at 8th and Spruce was 'way out in the country. Now it is in the center of a city, but the area still remains dominated by medical institutions.
In 1751, the Pennsylvania Hospital at 8th and Spruce was 'way out in the country. Now it is in the center of a city, but the area still remains dominated by medical institutions. Grievances provoking the American Revolutionary War left many Philadelphians unprovoked. Loyalists often fled to Canada, especially Kingston, Ontario. Decades later the flow of dissidents reversed, Canadian anti-royalists taking refuge south of the border.
Grievances provoking the American Revolutionary War left many Philadelphians unprovoked. Loyalists often fled to Canada, especially Kingston, Ontario. Decades later the flow of dissidents reversed, Canadian anti-royalists taking refuge south of the border.

