Related Topics
Old Age
New topic 2019-04-09 16:04:33 description
Old Age, Re-designed
A grumpy analysis of future trends from a member of the Grumpy Generation.
Philadelphia Places
New topic 2017-02-06 20:19:14 description
Retirement Communities (CCRC)
Let's confess my meager authority to generalize about trends in retiree convalescence. When I graduated from medical school in 1948, average American longevity was twelve or fifteen years shorter than today, and most assumptions rested on it's remaining the same forever. Someone who reached eighty was really old, obviously facing a prompt decline. Today, essentially everybody lives to be eighty. We only half-expect such long life, which is modest of us, and only halfway plan for it, which is foolish.
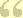 Picking the right CCRC is as hard as picking the right spouse. 
|
In 1950 a general practitioner in Haddonfield, NJ called for help from the son of one of his patients. The son was a doctor on the staff of the Pennsylvania Hospital, where I was finishing my internship. The GP hadn't had a vacation for twenty years and wondered if one of the graduating internets might take his practice for a month. I volunteered and then learned about retirement in a prosperous suburb. My employer had many tasks, among them a schedule of ten or twenty monthly house calls. There may have been some male patients on those rounds, but all I remember were old ladies living on the third floors of big old houses. I wasn't expected to do very much when I visited, at least by Emergency Room standards in the hospital. The families with whom the grandmothers were living wanted to be reassured that nothing was neglected. They also wanted to form their own assessment whether the doctor really knew them, and would come immediately if needed.
|
| Doctor House Call |
My next insight came a few months later when another doctor on the staff of the hospital had a heart attack; the Chief of Medicine gave me the time off to take care of this practice while the doctor recovered. When I first arrived at the door of the brick Philadelphia row-house where the doctor had his office, I was met by his nurse already wearing a raincoat, handing me an umbrella. We visited ten or fifteen other row houses along the neighboring streets, where to my amazement I found patients with oxygen tents and intravenous infusions. If the patients needed blood tests or electrocardiograms, the nurse arranged for them to be performed at home. Drugs by injection were administered, hospital-like bedside charts were maintained. This was a working-class neighborhood substitute for hospital care, but I was astonished to see how adequate it was. By this time, we had many resident physicians at the hospital who had seen service in the war and returned for specialty training; they regaled us at the lunch table about treating major illnesses -- in a tent. This wasn't the Civil War we were talking about, it was 1950.
Fifteen or twenty years later, my personal situation had improved; Medicare had arrived in 1965, but I was in practice as a center-city specialist and hardly noticed the new insurance system. But I did have three patients who insisted on being treated at home, which even by then had become an unusual arrangement. All three lived in condominium apartments in buildings with dining rooms on the main floor which would send up take-out dinners. All three patients had live-in nurses and hospital beds rented from an agency. One spinster lady absolutely refused to be treated in a hospital, because the Queen of England set up a little hospital in her palace when she needed it, and this lady said for practical purposes she had as much money as the Queen. Because she was dying of cancer, I resisted this idea, but if you had seen Katherine Hepburn in The Philadelphia Story you got the helpless feeling this dame was going to have her way. We called in laboratory and x-ray services as needed, administered injections, maintained a hospital chart. In this case, when I made a house call, her chauffeur would pick me up and deliver me, helping to ensure my promptness. Her lawyer and I kept careful financial records of the experience, which was new to him, too. After she died, we totaled it up and discovered with astonishment that the whole thing had been cheaper, a lot cheaper, than going to the hospital. Since she left a sum to the hospital in her will, even the hospital was pleased.
Well, nowadays there are more than fifty retirement communities scattered around the periphery of Philadelphia, many or most of them sponsored by Quakers. It's a national movement, and there are people in California who feel they had the idea first. There are now enough of these organizations to permit some classification of them into types, which mostly follows the sort of community model they resemble. There are some that look and are run like college dormitories, some that resemble convalescent homes, some are very like big-city apartment condos, and some behave like resort hotels. One of them, the Kearsley, sits in the middle of the Bala golf course, attempting to provide the first-class service to indigents by using existing government assistance programs, but has lately had to fall back on the Episcopal Church for financial help.

|
| CCRC |
Since a financial shadow hangs over all of them, it should be mentioned first. Every person in a retirement village is eligible for Medicare and Social Security, and with the help of a social worker can fall back on less-known assistance programs. It's impossible to ignore the existence of these funds, but most unwise to depend on them. As the age and number of retirees constantly grow, state and federal governments are starting to draw back from initial generosity. Laws have passed that a CCRC resident may not be evicted for non-payment of debts, so the institutions have had to impose conditions which guarantee them payment from new entrants in the case of later inability to pay. The risk remains that clients who entered before the rules were imposed, can only be extricated by going before Congress and raising a piteous cry on bended knee. Such laws and embarrassments vary from state to state, and from year to year, but unstable finances destabilize any business. When the customers all depend on their savings, and average investment experience is a drop of 30-50% in the past couple of years, no one escapes anxiety.
Although there must be college courses in how to administer a CCRC by now, current administrators are drawn from the environment the place mostly resembles, so the resemblance gets stronger. The former manager of a country club tends to neglect the infirmary; the former directress of a convalescent home doesn't notice institutional food. If the administrator treats customers as complaining nuisances, you get one kind of war; if the board of directors is accustomed to ruling corporations by dictate, you get another. Mainly, these institutions differ from models of other institutions by the degree to which they have active volunteers in charge. The inmates may run the asylum, but only if they become useful volunteers. A curious distinction evolves between those CCRCs which emerge from college alumni associations and those which are sponsored by churches. University faculties are not accustomed to, nor generally sympathetic with, teamwork. Every faculty member is on his own career path, which he hopes leads straight upward; teamwork to them is a code term used by business executives to imply blind obedience, Charge of the Light Brigade, or worse. Church groups, on the other hand, prize volunteerism. In a church environment, the proposal that Let's Have a Picnic is supposed to be met with a chorus of Great, I'll be Glad to Bake a Cake. Church-sponsored CCRCs, therefore, are generally more adaptive to innovation in a formless society. University groups have camaraderie and complaining, but little follow-through. By contrast, business people know what you are supposed to do, you are supposed to make something happen. Church volunteers want to know how they can help. Paradoxically for that reason, the more evidence of golf clubs around the place, the more likely it is to be innovative.
Let's return to the point, succinctly. Life-threatening and potentially convalescence-requiring medical conditions are destined to segment increasingly into Medicare, to the point where what remains outside of Medicare is elective, preventive or outpatient. Obstetrics is an exception, remaining more naturally part of the hospital than the CCRC. The rest of medical care thus seems inclined to migrate toward the suburban ring of retirement communities. The more natural transportation flow is for younger people to travel to either a hospital-centered medical cluster or a CCRC-centered cluster, not for frail old folks to leave the convalescent environment except for major surgeries from which they soon return to their infirmary. It doesn't have to be that way, it just seems like the natural arrangement.
Probably the main reason it doesn't work that way today resides in the Medicare law. The 1983 amendments restrained inpatient reimbursement much more than outpatient care or home nursing care, and consequently, inpatient costs have risen 18% in five years, compared with 47% for outpatient. Outpatient care is not migrating toward retirement communities because hospitals need revenue. Somehow, it seems easier to modify these reimbursement rules than to upend suburban CCRCs and relocate them next door to an urban hospital. If the payment rules become reasonable, the system will readjust its geography in a reasonable way, without coaxing.
Surely, non-residents of the CCRCs are destined to wish to convalesce in the spare beds of CCRC infirmaries which should then treat younger people as a much-needed revenue source; any licensing requirements which block this seem unreasonable. Medical hardware,-- x-rays, MRIs and the like,-- is most naturally concentrated in the periphery of CCRCs, as are pharmacies, outpatient labs, doctors' offices. That's going to require a lot of parking space. It's a good thing this will take a couple of decades to happen; many mid-course adjustments will be imperative. But the basic fact is that the whole community's medical need is getting concentrated in CCRCs via Medicare, and so the community's facilities should move closer to that need. The younger community is well able to travel anywhere for elective medical services, especially when they move away. Makes a good chance to visit the grandparents while they are there, too.
All of these proposals depend on getting the attention and cooperation of other self-centered institutions: Medicare, hospitals, medical societies, municipal governments. The CCRC community has scant experience with asserting itself; its future will depend on how skillfully it begins to do so.
Nearly every retirement village has four or five retired physicians living in the place, as well as a dozen retired nurses, lab technicians, and others with medical experience. Every CCRC infirmary has four or five patients whose spouse is a resident of the community, visiting the infirmary regularly, and with sharpened insight. Some other people are natural leaders. If these people could be assembled into a permanent committee of medical oversight, charged with visiting other CCRCs in the region for ideas and perfecting the interface between the CCRC and nearby hospitals, medical facilities, transportation vendors, and politicians -- things would start to move. Spending twenty percent of our gross domestic product on health is, quite enough. Let's either stop spending so much or else make something good of it.
Originally published: Thursday, July 16, 2009; most-recently modified: Thursday, May 02, 2019